Canine Pancreatitis: A Dog Owner's Guide to Symptoms, Treatment & Recovery
Let's talk about something that scares a lot of dog owners: pancreatitis. It's not just a tummy ache. When your dog's pancreas gets inflamed, it's a serious, painful condition that needs immediate attention. I've seen too many cases where well-meaning owners missed the early signs, thinking it was just a bit of indigestion. The truth is, understanding pancreatitis can be the difference between a quick recovery and a life-threatening emergency.
This guide cuts through the jargon. We'll cover what pancreatitis actually is, why certain dogs are ticking time bombs for it, and the specific signs you should never ignore. More importantly, we'll walk through exactly what happens at the vet, the reality of treatment costs, and how to build a long-term management plan that actually works. Consider this your roadmap for navigating one of the most common yet misunderstood canine health crises.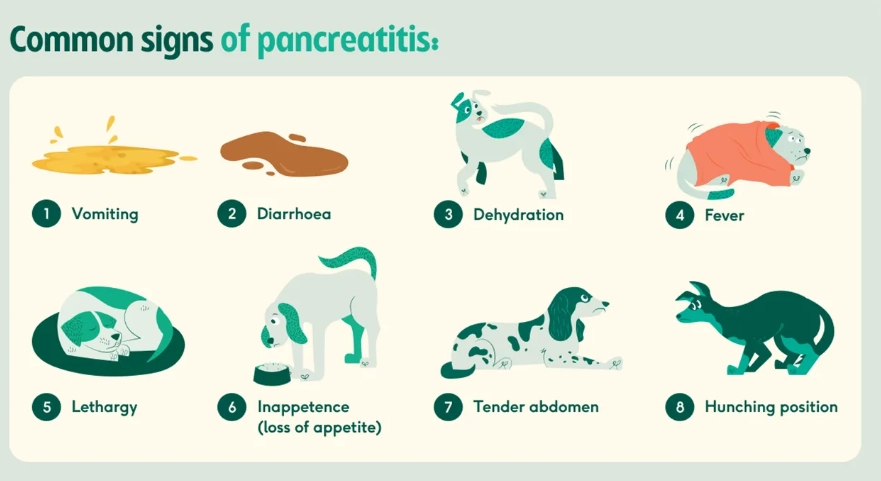
What You'll Find in This Guide
- What Exactly Is Pancreatitis in Dogs?
- Symptoms & Signs: Is It Pancreatitis or Just an Upset Stomach?
- Causes & Risk Factors: Why Did This Happen to My Dog?
- Diagnosis: What to Expect at the Vet's Office
- Treatment Options for Canine Pancreatitis
- The Recovery Phase & Long-Term Diet Management
- Prevention Strategies for High-Risk Dogs
- Your Pancreatitis Questions Answered
What Exactly Is Pancreatitis in Dogs?
The pancreas is a small organ near the stomach with two big jobs: producing insulin to regulate blood sugar, and producing digestive enzymes to break down food. Pancreatitis occurs when those digestive enzymes are activated too early—while still inside the pancreas—and begin literally digesting the organ itself. It's as painful as it sounds.
Vets classify it as either acute (sudden and severe) or chronic (ongoing, lower-grade inflammation). Acute episodes are medical emergencies. Chronic pancreatitis is more of a smoldering fire, causing gradual damage and often leading to conditions like diabetes or exocrine pancreatic insufficiency (EPI) over time.
Symptoms & Signs: Is It Pancreatitis or Just an Upset Stomach?
This is where owners get tripped up. The signs can mimic simple gastroenteritis. But the intensity and combination are different. Here’s what to watch for, ranked from most common to more subtle.
The Classic Triad: Vomiting, abdominal pain, and loss of appetite. The pain isn't just whining. A dog with pancreatitis often adopts a "praying position"—front legs down, rear end up—to relieve pressure on its belly. They might flinch or growl if you gently press the area just behind the rib cage.
Other Key Symptoms:
- Lethargy that's more profound than usual tiredness.
- Fever.
- Diarrhea, which may be yellowish and greasy.
- Dehydration (check for sticky gums).
- A hunched back.
If your dog exhibits the classic triad, especially after getting into fatty food, treat it as urgent. Don't wait to see if it "passes."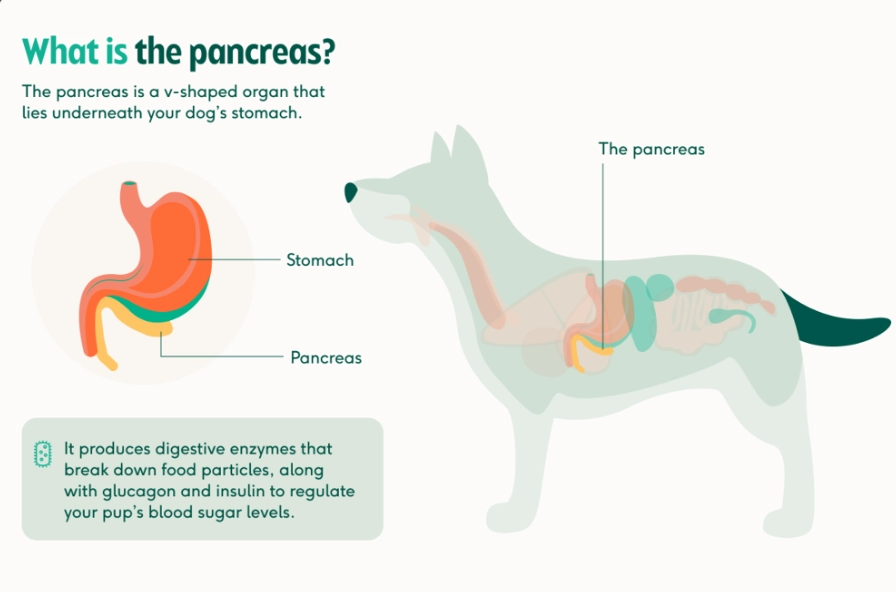
Causes & Risk Factors: Why Did This Happen to My Dog?
It's rarely one thing. Think of it as a perfect storm. The most common trigger is dietary indiscretion—the Thanksgiving turkey skin, the greasy burger patty stolen off the grill, the entire stick of butter left on the counter. But that's just the spark.
The underlying fuel often includes:
| Risk Factor | Why It Matters | Common Breeds/Profiles |
|---|---|---|
| Breed Predisposition | Genetics play a huge role. Some breeds have metabolisms prone to high triglycerides or sensitive pancreases. | Miniature Schnauzers, Yorkshire Terriers, Cocker Spaniels, Shetland Sheepdogs. |
| Obesity | Excess fat tissue promotes systemic inflammation and strains organ function. | Any overweight dog, but especially those on high-fat diets. |
| Underlying Conditions | Other diseases can stress the pancreas or alter fat metabolism. | Dogs with Cushing's disease, diabetes, hypothyroidism, or epilepsy (on certain medications). |
| Chronic High-Fat Diet | Consistently feeding fatty table scraps or high-fat kibble keeps the pancreas working in overdrive. | Dogs fed "people food" regularly or on inappropriate commercial diets. |
| Trauma or Surgery | Physical injury near the abdomen can directly damage the pancreas. | Dogs hit by cars, falling from heights, or recent abdominal surgery. |
I once treated a Miniature Schnauzer named Bailey who had three acute episodes in a year. The owner was meticulous with diet. Turns out, Bailey had a hidden, genetic lipid disorder. The standard advice wasn't enough; he needed specialized medication to manage his blood fats. This is why identifying your dog's personal risk profile is crucial.
Diagnosis: What to Expect at the Vet's Office
There's no single, perfect test for pancreatitis. Diagnosis is a puzzle, and your vet will piece it together. Expect a combination of the following:
1. Physical Exam and History
Your vet will palpate the abdomen and ask detailed questions: "What did he eat in the last 48 hours? Any access to garbage? Any recent dietary changes?" Be brutally honest about table scraps.
2. Blood Work
This is essential. They'll look at:
Pancreatic Lipase Immunoreactivity (cPLI or SPEC cPL): This is the gold-standard blood test. It's highly specific for pancreatic inflammation.
Complete Blood Count (CBC) & Chemistry Panel: To check for dehydration, infection, elevated liver enzymes, and electrolyte imbalances.
Triglyceride Levels: Especially important in breeds like Schnauzers.
3. Diagnostic Imaging
Abdominal Ultrasound: This is the most useful imaging tool. A skilled technician can often see an enlarged, inflamed pancreas and rule out other causes like a foreign body or tumor. It's non-invasive and provides a lot of information.
X-rays might be taken first to rule out an obstruction, but they often appear normal in pancreatitis cases.
Treatment Options for Canine Pancreatitis
Treatment depends entirely on severity. Mild cases might be managed at home with strict rest and a vet-prescribed diet. Moderate to severe cases require hospitalization. Here's the standard hospital protocol:
Aggressive Fluid Therapy: This is the cornerstone. IV fluids combat dehydration, maintain blood pressure, and help flush out inflammatory toxins. This is often the most critical part of treatment.
Pain Management: Pancreatitis is excruciating. Dogs will receive strong pain relievers (like opioids) and anti-nausea medication. Ignoring pain slows recovery and is inhumane.
Nutritional Support: The old-school approach was to withhold all food and water (NPO) for days to "rest" the pancreas. Modern veterinary medicine, as supported by resources like the Merck Veterinary Manual, has shifted. We now know early, gentle feeding with a highly digestible, low-fat diet can actually improve outcomes and prevent complications. This might mean a feeding tube placed directly into the small intestine, bypassing the stomach, to deliver nutrition without stimulating the pancreas too much.
Antibiotics: These are used only if there's evidence of a secondary bacterial infection, which can happen if the inflamed gut lining becomes leaky.
Cost is a real concern. Hospitalization for severe pancreatitis can range from $1,500 to $5,000 or more, depending on location and complications. Pet insurance that covers illness can be a lifesaver here.
The Recovery Phase & Long-Term Diet Management
Your dog comes home. Now what? This phase is where most long-term success or failure is determined.
The First Few Weeks: Your vet will prescribe a veterinary therapeutic low-fat diet (like Royal Canin Gastrointestinal Low Fat or Hill's i/d Low Fat). Stick to it religiously. No treats, no scraps. I mean it. The pancreas needs months, not weeks, to truly calm down. Re-introducing fat too soon is the fastest way to trigger a relapse.
Building a Long-Term Diet: After a few months, you might transition to a high-quality, commercial low-fat maintenance diet. Look for foods where fat is less than 10% on a dry matter basis. Your vet can help you calculate this.
Safe Treat Alternatives: This is a major pain point for owners. You have options:
- Commercial low-fat treats (check the label).
- Plain, boiled, skinless chicken breast (shredded).
- Green beans or carrots (steamed, no butter).
- Small pieces of apple or banana.
A common mistake I see is owners switching to a "sensitive stomach" formula that's still high in fat. Read every label. "Grain-free" often means higher fat from alternative starches like peas and potatoes.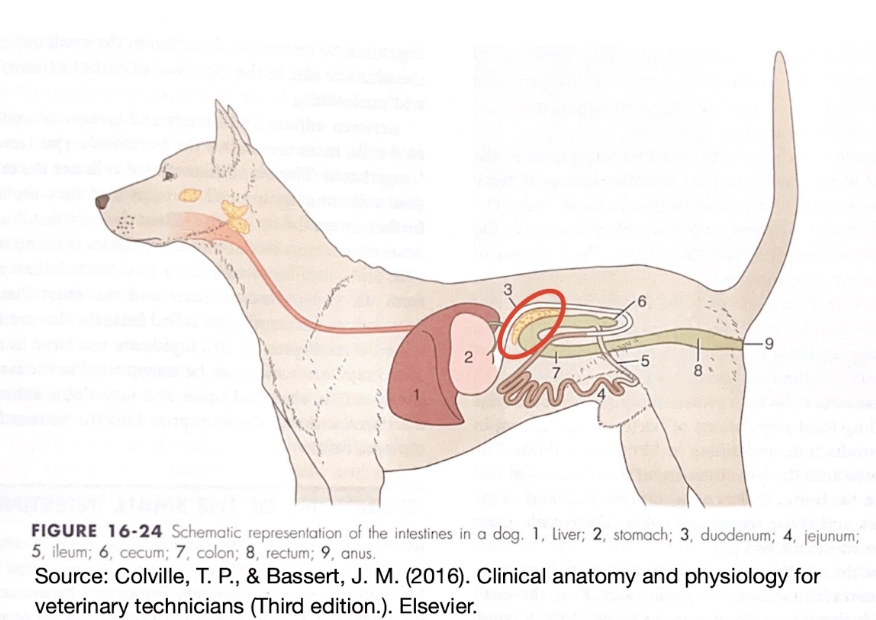
Prevention Strategies for High-Risk Dogs
If your dog has had pancreatitis once, prevention becomes your daily mission.
Diet is Everything: Commit to a lifelong low-fat regimen. Measure meals. Avoid all high-fat human foods permanently. This isn't a punishment; it's a necessary medication.
Weight Management: If your dog is overweight, work with your vet on a safe weight loss plan. Even losing 10% of body weight can dramatically reduce inflammation.
Manage Underlying Conditions: Ensure any other diseases (like hypothyroidism) are well-controlled with medication.
Be Vigilant: Know the early signs. You're now an expert. At the first hint of lethargy or reduced appetite, you can act fast.
Your Pancreatitis Questions Answered
 My vet said my dog's blood work shows "mild pancreatitis." Does this need treatment, or can I just watch him at home?
My vet said my dog's blood work shows "mild pancreatitis." Does this need treatment, or can I just watch him at home?Pancreatitis is a tough road, but with swift action, dedicated aftercare, and a committed change in lifestyle, most dogs can recover and live full, happy lives. Your awareness is their best defense.